Please note: for the purposes of today’s post, we’ll be talking about chronic pelvic pain for folks with vaginas.
What is Chronic Pelvic Pain?
Chronic pelvic pain is pain that lasts for more than six months in the pelvic area.
This pain can be experienced constantly, on a regular cycle, or only at certain times. For example, you might only experience this pain when menstruating, emptying your bladder, during or after sexual intercourse, or from sitting or standing for long periods of time.
Although chronic pelvic pain is very common, with as many as 25% of women experiencing this at some point in their lives, there’s been a lack of research into the exact mechanisms of chronic pelvic pain.
What Does Chronic Pelvic Pain Feel Like?
Chronic pelvic pain can be felt in different areas of your pelvis, not just one spot every time. Chronic pelvic pain can be mild to moderate or be so intense they might cause you to miss work or prevent you from living the way you prefer.
Chronic pelvic pain can be described in several ways including:
- Pressure or heaviness in the pelvis
- Dull aching
- Serious and steady
- Pain that comes and goes
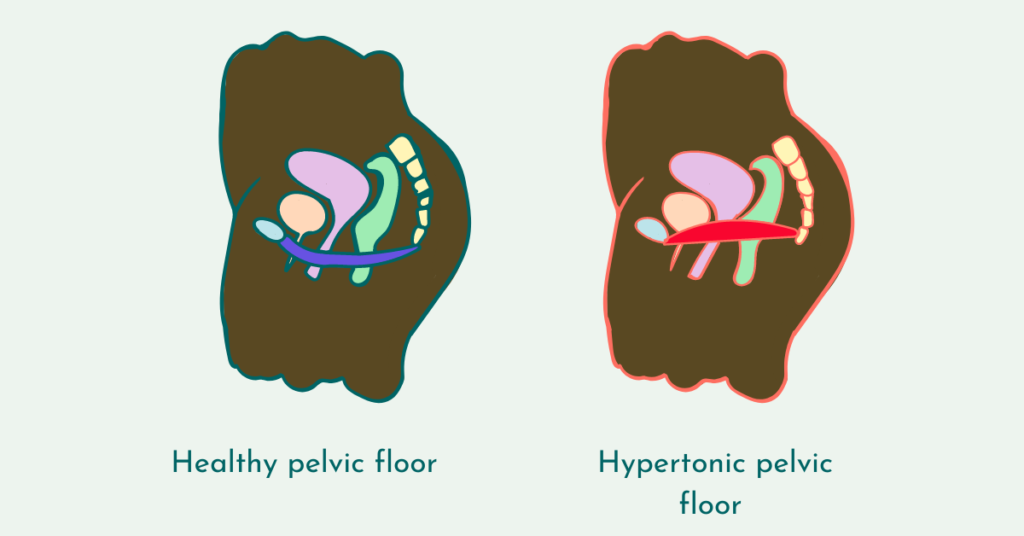
Because many of the conditions leading to chronic pelvic pain cause your pelvic floor to become too tight or tense up (hypertonic) and the pelvic floor acts as a hammock that supports your organs including your bowel, bladder, and uterus you may also experience symptoms like:
- An urgent or frequent need to urinate
- Abdominal bloating
- Gastrointestinal problems like upset stomach or IBS
- Constipation
What Causes Chronic Pelvic Pain?
There are a range of conditions that can cause chronic pelvic pain and it’s important that you see a healthcare provider as soon as possible when you start experiencing symptoms.
Some conditions that cause chronic pelvic pain include but are not limited to:
- Endometriosis
- Side effects from radiation in your pelvic area (radiation induced vaginal stenosis)
- Uterine fibroids
- Pelvic inflammatory disease
- Pelvic floor injury caused by an accident, pregnancy, or childbirth
- Interstitial cystitis, also known as painful bladder disease
- Dysmenorrhea (painful periods)
How is Chronic Pelvic Pain Treated?
The first step to treating chronic pelvic pain is seeing a healthcare professional who will take a medical history, ask you about your daily life, and conduct a pelvic exam.
Depending on your diagnosis the underlying condition may be treated with medication for infection, hormonal birth control for issues with menstruation, or potentially surgery.
For many people with chronic pelvic pain, managing the pain and severity is achieved through:
- Pelvic Floor Physiotherapy – Pelvic floor physiotherapists (or PFPTs) work to help you rehabilitate your pelvic floor muscles. They are specially trained to conduct internal and external assessments and treatments for your pelvic floor. Learn more about what to expect from your first pelvic floor physio appointment. [link to blog]
- Vaginal dilators – Vaginal dilators (inserts) are plastic or silicone rods or cylinders with a rounded tip. They are meant to open (dilate) and stretch the tissues of the vagina.
- Cognitive behavioral therapy or sex therapy – this does not mean that your pain is not real or “all in your head” but rather, a licensed professional may help to support you through your treatment plan
Hyivy Health is currently working with researchers across the world to help grow our knowledge base of how chronic pelvic pain works and how to better treat it. We’re currently developing a smart vaginal dilator with multi-therapy capabilities which will be the first ever to collect both subjective and objective data on the pelvic floor which will be shared with clinicians through our clinician software.
If you or someone you know is interested in participating in focus groups and potential product testing, reach out today.
—
Is there a blog topic you’d like us to cover? Reach out today to let us know.
Here at Hyivy Health we’re dedicated to helping women down there and everywhere. The purpose of this blog post is intended to offer resources and education about pelvic health and is not intended to serve as medical advice. This information provided above is not a substitute for the treatment, advice, or opinion of a medical professional. Always consult with a certified health professional before starting any treatments.