What is the Pelvic Floor?
The pelvic floor is a group of muscles that stretch from the tailbone (also known as the coccyx) to the pubic bone at the front and between the sitz bones from one side to the other.
Think of your pelvic floor as a hammock just under your core, making sure everything stays in place. The 36 muscles that make up your pelvic floor all work to support pelvic organs like the vagina, cervix, uterus, bladder, urethra, uterus, prostate, and rectum.
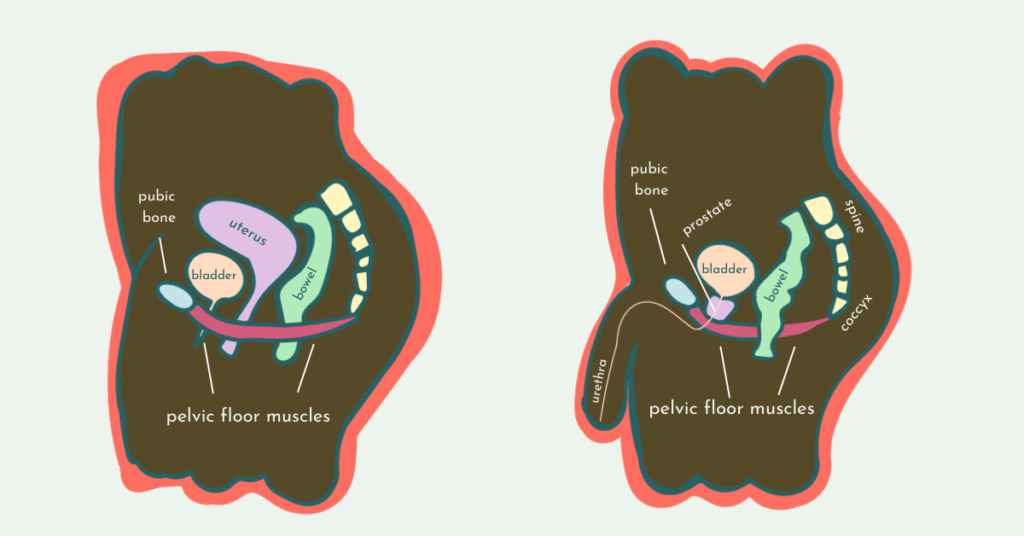
The pelvic floor muscles are like a hammock supporting all of your pelvic organs
What does the Pelvic Floor do?
The pelvic floor muscles provide the main support for the pelvic organs, but serve multiple other functions, including:
- Urinary continence
- Fecal continence
- Sexual intercourse
- Orgasms and erections
- Vaginal delivery during childbirth
The pelvic floor isn’t an isolated group of muscles that handle going to the bathroom and reproduction and sexual function. Pelvic floor muscles also provide stability for your core and involve complex coordination between somatic and autonomic motor nervous systems. Somatic motor functions are voluntary actions like standing or sitting, and autonomic motor functions are involuntary like breathing or blinking.
For example, you don’t have to think about the pelvic floor muscles that are working together to keep your pelvic organs like your bladder or uterus in place. But now think about stopping urine midstream when you’re peeing – those are some of your pelvic muscles at work.
Now imagine you’re trying to pick up a cherry from the floor with your pelvic floor muscles. You’re going to have to voluntarily squeeze some of them, right? (You’re also probably never going to look at a cherry the same way again!)
Hyivy Health’s 5 Pelvic Floor Vital Signs
The purpose of this list is to give you a sense of the various ways your pelvic floor can be thought about, felt, monitored, and cared for:
1. Sensation
The pelvic floor has a wide range of physical reactions and sensations, including sexual response and orgasm. The symptoms to look out for when you may need to consult a clinician are: chronic pain (pain that continues for more than three months), loss of libido, inability to achieve arousal, or discomfort.
2. Lubrication
The level of moisture in the pelvic floor is subject to hormonal changes and there is a unique level of discharge and lubrication for every individual.
The symptoms to look out for when you may need to consult a clinician are: irregular discharge including watery consistency, abnormal color, or increased frequency, and chronic vaginal dryness (dryness that continues for more than three months).
3. Incontinence
The pelvic floor is responsible for both urinary and bowel control.
The symptoms to look out for when you may need to consult a clinician are: pain with urination, increase in urinary frequency (overactive bladder), or loss of urinary or bowel control.
4. Health of tissues
Usually, we don’t notice the health of tissues until something is wrong.
The symptoms to look out for when you may need to consult a clinician are: stenosis (narrowing and shortening of the vagina), sores and rashes, thinning of the skin in the vagina or on the vulva, redness, irritation, itching, bleeding, or atrophy.
5. Muscle control and response
The inability to correctly relax and coordinate your pelvic floor muscles is called pelvic floor dysfunction.
The symptoms to look out for when you may need to consult a clinician are: pelvic muscle weakness (hypotonic) and overactive pelvic muscles (hypertonic). For more in-depth details on these symptoms, check out our blog post on the difference between a hypertonic and hypotonic pelvic floor.
—
Is there a blog topic you’d like us to cover? Reach out today to let us know.
Here at Hyivy Health, we’re dedicated to helping you down there and everywhere. The purpose of this blog post is to offer resources and education about pelvic health and is not intended to serve as medical advice. The information provided above is not a substitute for the treatment, advice, or opinion of a medical professional. Always consult with a certified health professional before starting any treatments.